
Managing Sustainable Public Health Data Exchange at the National Level
The pandemic taught many lessons about public health infrastructure. Among them, that rapid scale-up in response to emergencies is only sustainable when paired with a platform that can agilely connect public health systems and healthcare providers across the country. And this national network generates massive volumes of data, which translates into substantial operational costs.
A Robust Foundation
The APHL Informatics Messaging Services (AIMS) Platform has long served as the backbone of national public health data exchange, processing more than 40 million messages per month across laboratories, federal partners, hospitals, and other public health collaborators. Think of it as a high-speed interstate transporting critical information—surveillance messages, electronic case reporting (eCR), immunization data, vital statistics, electronic laboratory results (ELR), electronic test orders and results (ETOR), and other public health reporting—from one point to another. By centralizing these intermediary services into a single platform instead of replicating efforts across every public health jurisdiction, AIMS saves money, time and lives.
But with great success comes great operational complexity. When COVID-19 hit, the platform scaled dramatically to meet demand. For example, in late 2020 AIMS processed about 2.15 million initial electronic case reports (eICR) per month. But by the end of 2024, AIMS was processing more than 26 million eICR per month, with numbers continuing to increase. Other use cases saw similar increases in activity during the same period. That exponential increase in message volume brought a corresponding spike in operational costs in the form of monthly bills from Amazon Web Services (AWS).
Growth in Monthly eICR Volume Processed on AIMS (2020–2024)
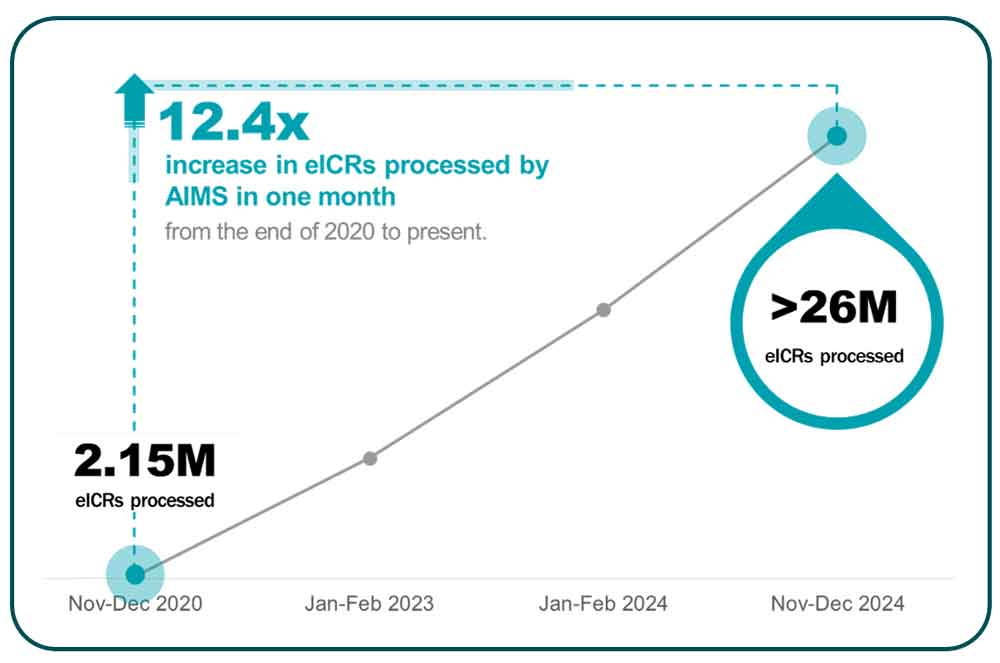
After the emergency ended, the volume of data continued to increase as more conditions and healthcare organizations onboard and as AIMS evolved to handle more use cases. For example, the platform recently assumed responsibility for reporting ELR to jurisdictions from the US Centers for Disease Control and Prevention’s (CDC’s) ReportStream and SimpleReport. CDC also commissioned APHL to build and operate Detor, a centralized, fast and secure system to transmit ETOR between healthcare systems and public health collaborators. Already, more than 100,000 newborn screening, sexually transmitted infection (STI) and tuberculosis (TB) orders and results have been exchanged through Detor since the service went live in August 2024, saving hundreds of hours for both hospitals and laboratories, reducing turnaround time by days and potentially saving lives. These expansions to AIMS demonstrate its versatility and CDC's continued reliance on and trust in the platform.
AIMS gets the job done, but at a cost. As funding tightens across public health, APHL is trying to find ways to reduce expenses. This public health intermediary will only be sustainable if it can streamline its operations and make the investment more cost-effective.
The Stabilization Initiative
This past year, APHL focused on stabilizing and streamlining operations across the AIMS Platform. The association overhauled how messages are processed and routed without disrupting services to users—no small feat when the platform is handling 480 million annual messages that healthcare organizations, laboratories and agencies depend on at the local, state and federal level. Through careful process improvement efforts, the platform achieved considerable reductions in operating costs while maintaining the same level of service reliability.
The work began with comprehensive analysis. The team leveraged AWS tools including Cost Explorer, Compute Optimizer and Trusted Advisor to generate data-driven insights about where resources were being consumed. They established a semi-permanent governance structure to continue process improvements and identify additional savings opportunities. Every system component came under scrutiny.
One way that APHL has reduced costs and overhead is by leveraging cloud native services where possible. For example, a fully managed, scalable service is now used (AWS Transfer Family) that reduces the maintenance burden, and cloud governance solutions and rules are being implemented to reduce overhead on APHL
Another major milestone was completing the Mirth Resilience project. While the primary goal was improving performance, resource utilization, and scalability within the electronic case reporting architecture, an additional benefit emerged: message processing and storage efficiencies that correlated to significant AWS cost reductions. Even after only one month in production, these cost savings were apparent in the monthly invoices.
The results speak for themselves. Current cost-saving efforts have resulted in approximately $258,000 per month in reductions. It is important to note that savings don't always show up as a direct one-to-one drop in monthly invoices—sometimes unused resources are removed only to add resources for another workload. But the net effect remains a positive reduction.
Looking Ahead: The Volume Challenge
Cost stabilization doesn't mean the work is done. APHL is already exploring the next frontier: reducing the volume of eCR messages themselves. A significant portion of what healthcare organizations currently send to AIMS cannot be used by public health agencies. These non-reportable eICRs still require processing and routing, which drive costs.
Several enhancement strategies are under consideration. One straightforward approach would remove high-volume conditions that produce substantial electronic case reporting loads but have minimal or no Reportable Condition Knowledge Management System (RCKMS) authoring by public health agencies. Malignant neoplastic disease represents one such condition. The impact could be substantial: filtering these non-reportable cases could result in an estimated 25 to 30 percent volume reduction, with corresponding operational savings from reduced ingestion, processing and routing.
A Platform for the Future
This stabilization work positions AIMS to support public health through funding uncertainties while preparing for the platform's next evolution. APHL is constantly looking ahead, seeking partners throughout the health IT ecosystem to develop and pilot new use cases for TEFCA, FHIR and the CMS Interoperability Framework. Through this innovation, AIMS will be ready when public health needs reliable data exchange solutions.
The pandemic proved that public health infrastructure can scale rapidly to meet unprecedented challenges. The AIMS stabilization initiative proves something equally important: that careful stewardship and strategic thinking can ensure those systems remain sustainable for the long haul. As public health faces an uncertain funding landscape, this kind of financial discipline will be essential to maintaining the critical services the nation depends on.

